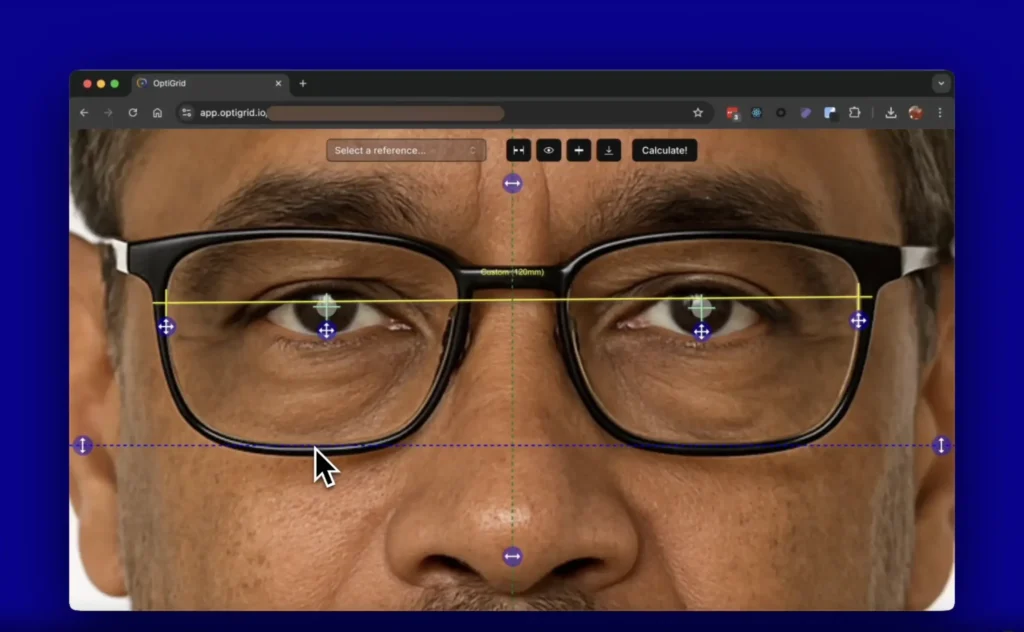
A digital PD ruler measures pupillary distance using a camera and software instead of a manual ruler or pupillometer. Peer-reviewed studies show that the best smartphone-based PD apps achieve a mean absolute error of roughly 0.5 mm compared to a digital pupillometer, putting them within the tolerance range that most lens manufacturers accept. For opticians evaluating these tools, the practical question is whether a given digital workflow is consistent enough to reduce remakes and support remote eyewear orders without sacrificing fitting accuracy.
This guide covers how digital PD rulers work, what published accuracy data actually shows, how they compare to traditional methods, and what to consider before adopting one in a clinical or retail optical setting.
How Pupillary Distance Measurement Has Changed

From Manual Rulers to Camera-Based Tools
Pupillary distance has traditionally been measured with a millimeter ruler held across the bridge of the nose, or with a corneal-reflection pupillometer like the TOPCON PD-5. Both methods work, but they depend heavily on the operator’s technique and consistent patient positioning.
Digital PD tools emerged as more eyewear dispensing moved online and as multi-location practices looked for ways to standardize measurements across staff. A 2024 comparative study in Clinical Optometry found that PD ruler measurements overestimated distance IPD by a mean of 0.54 mm compared to a pupillometer, partly due to Angle Kappa, the difference between the pupillary axis and the visual axis. Digital tools that use corneal reflection detection can reduce this specific source of error.
With tools like Optogrid, practices can use a photo-based workflow to support remote eyewear sales and standardize optical measurements across locations. For a broader look at how measurement technology is reshaping online optical retail, see Measurement Technology Driving Online Optical Retail Growth.
How Digital PD Rulers Work
Digital PD rulers estimate the distance between pupils using a camera (phone, tablet, or dedicated device) plus software. The process involves two core tasks: detecting facial and eye landmarks reliably, and converting pixels into millimeters using a known reference or calibrated setup.
A typical measurement follows these steps:
- The patient positions themselves in front of the camera at a specified distance.
- The device prompts the patient to look at a fixed point for alignment.
- The camera captures an image of the patient’s face.
- Software identifies the pupils (or corneal reflections) and calculates the distance between them.
- The PD measurement displays, often within seconds, sometimes with a quality or retake warning.
Compared to a manual ruler, digital tools offer more consistency and speed. The tradeoff is sensitivity to positioning, camera quality, lighting, and whether the method includes a reliable scaling reference.
Digital PD Accuracy: What the Research Shows
Accuracy is the question that matters most, and it is also where marketing claims often outpace evidence. Published comparative studies give a clearer picture.
A 2023 study in Cureus comparing three smartphone apps (PDCheck AR, Eye Measure, and Warby Parker) to a digital pupillometer across 44 subjects found that the Warby Parker app achieved the lowest mean absolute error at 0.51 mm. The study concluded that when patients cannot receive IPD measurements from trained clinicians, validated smartphone apps “may serve as an acceptable alternative.”
A 2024 study in Clinical Optometry comparing a pupillometer, PD ruler, autorefractor, and the Eye Measure mobile app across 40 participants found all methods stayed within the ISO 16034:2002 spectacle manufacturing tolerance of 0.33 prism diopters. The mobile app showed a mean difference of -0.59 mm from the pupillometer for distance IPD, while the PD ruler showed +0.54 mm.
The practical takeaway: validated digital PD tools can produce measurements within clinically acceptable tolerances, but accuracy varies by app and depends on capture conditions. Any adoption should include testing against your baseline method and documenting when fallback to manual measurement is needed.
PD Measurement Method Comparison
| Method | Typical Accuracy (vs. Pupillometer) | Speed | Cost | Best For |
|---|---|---|---|---|
| Manual PD Ruler | +0.54 mm mean difference | 30-60 seconds | Under $10 | Budget-conscious practices, backup method |
| Digital Pupillometer | Gold standard (reference) | 15-30 seconds | $500-$2,000+ | High-volume dispensing, clinical baseline |
| Smartphone App | 0.5-1.4 mm MAE (varies by app) | 10-30 seconds | Free to $50/month | Remote orders, patient self-measurement |
| Photo-Based Platform (e.g., Optogrid) | Calibrated with reference | 15-30 seconds | SaaS subscription | Multi-location standardization, remote dispensing |
Data sources: PMC10389117 (2023), PMC11654209 (2024). Accuracy figures reflect study conditions; real-world results depend on lighting, positioning, and user guidance.
Digital PD Tools in Clinical Practice
Adoption Patterns Across Practice Types
Digital PD tools are increasingly common in optometric and ophthalmologic settings, but adoption is not uniform. Practices adopt them for practical reasons: reducing chair time, supporting remote pupillary distance measurement workflows, and making measurements more repeatable across staff members.
Adoption patterns vary by practice type:
- Urban and multi-location practices: Higher adoption driven by demand for remote-friendly workflows and the need to standardize measurements across staff
- Rural practices: Gradual adoption as tools become simpler to deploy and support
- University-affiliated clinics: Often early adopters when the tool supports research or standardized protocols
- Independent optometrists: Adoption varies; many adopt digital tools when it helps them compete on convenience without losing measurement quality
For most practices, digital PD tools are about consistency, throughput, and fewer measurement-related remakes downstream.
How Digital PD Measurement Affects Patient Experience
Digital PD tools can improve the patient experience when they reduce friction. Instead of repeating measurements or struggling with a manual ruler, patients get a faster, more guided process.
- Guided capture: Good tools prompt the patient clearly and flag poor-quality captures
- Speed: Measurements complete in seconds once the workflow is familiar
- Comfort: Most approaches are non-contact, which many patients prefer
Accuracy still matters most. A smoother experience is not helpful if it increases remake rates. The goal is to make the process easier while keeping the measurement trustworthy.
What Successful Digital PD Adoption Looks Like
Practices that report positive outcomes with digital PD tools share common patterns: fewer measurement redos, clearer documentation, and smoother workflows for remote eyewear orders. Some also report fewer post-dispensing adjustments tied to measurement issues, especially when the digital workflow includes verification steps.
Digital PD tools work best when they are part of a structured process: capture, quality check, confirm, document. That sequence keeps convenience from turning into callbacks. Practices considering adoption should also look at how digital measurement fits into broader optical business workflows including inventory, ordering, and patient records.
It is worth tracking long-term outcomes: remake rate, returns, and how often staff switch to a fallback method. That data tells you whether the tool is genuinely helping or just shifting work around.
Computer Vision and AI in PD Measurement

What AI Actually Does in Digital PD Tools
In PD measurement, AI primarily shows up as computer vision: detecting eye landmarks reliably, handling imperfect captures, and flagging low-quality images. The 2024 comparative study noted that test-retest reliability was strong across all methods (r=0.9, p<.01), suggesting that when digital tools work well, they produce repeatable results.
The most practical AI contributions in current PD tools include:
- Automated landmark detection that makes PD capture more consistent across lighting conditions and face shapes
- Quality scoring that warns users when lighting, pose, or glare makes a measurement unreliable
- Reference calibration that converts pixel distances to millimeters using known objects (credit cards, specific frames, or printed markers)
AI is valuable when it improves reliability and catches bad inputs. If a tool cannot explain why it flagged a capture as poor quality, it will struggle to earn trust in clinical settings. As these tools mature, practices need clarity on how the tool was validated, what conditions affect performance, and what the recommended fallback is.
Where Ophthalmic Biometrics Is Heading
For eyewear dispensing, the practical next steps in digital measurement are better remote capture guidance, more consistent calibration methods, and clearer quality scoring so staff know when to trust a result. There is growing interest in combining multiple signals, including face geometry, gaze direction, and capture quality, to make measurements more stable across different phones and environments.
Eye care broadly is becoming more data-driven. Large clinical registries like the IRIS Registry (managed by the American Academy of Ophthalmology) reflect this trend: tools and treatments are increasingly expected to demonstrate measurable outcomes and evidence-based validation. For PD tools specifically, this means that practices will increasingly expect accuracy benchmarks, documented tolerances, and clear quality controls before committing to a workflow change.
Challenges in Adopting Digital PD Measurement

Building Trust Through Validation, Not Marketing
The biggest barrier to digital PD adoption is not technology but trust. Some practitioners have seen inconsistent app results or worry that staff will use the tool without proper technique. The 2023 study’s finding that app accuracy varied significantly, with mean absolute errors ranging from 0.51 mm to 1.38 mm depending on the app, underscores why validation matters more than vendor promises.
The best way to reduce skepticism is not with marketing claims, but with clear validation data, staff training, and defined rules for retakes and fallbacks. Start small: define your workflow, train staff, measure outcomes, and only then scale across the practice.
Privacy and Data Handling
Digital PD workflows often involve face images or biometric-like data, which raises real privacy and security questions. If a tool captures photos, stores them, or uses them to compute measurements, it needs clear policies and strong security practices.
- Transparent data protection measures and retention policies
- Access control mechanisms limiting who can view patient images
- Clear communication with patients about what data is collected and why
Patients generally accept digital capture when they understand what is being collected, how long it is kept, and who can access it. Any practice adopting digital PD tools should confirm applicable requirements (local health privacy laws, consumer privacy rules, and vendor contracts) and ensure staff know how to handle patient data safely.
Making Digital PD Tools Work Across Settings
Digital PD measurement can improve access, especially for remote patients, but only if the tools are practical across different devices and communities. Equity is not only about price; it also involves language, guidance quality, and the ability to capture a usable image in everyday conditions.
- Affordability: Pricing and hardware requirements should match the reality of small practices and budget-conscious patients
- Accessibility: Tools should work in varied environments, not just perfect lighting with the latest smartphone
- Training: Short, practical training and clear “when to retake” guidance make adoption smoother everywhere
To explore a photo-based workflow for optical measurements, access our app and explore OPTOGRID. Sign in to test how it fits into your dispensing process.
Frequently Asked Questions
What is a digital PD ruler and how accurate is it?
A digital PD ruler is a tool that measures pupillary distance using a camera and software instead of a manual ruler. A 2023 peer-reviewed study found that the most accurate smartphone PD apps achieved a mean absolute error of 0.51 mm compared to a digital pupillometer, which is within clinically acceptable tolerance for most eyeglass prescriptions.
How does a digital PD ruler compare to a pupillometer?
A pupillometer remains the gold standard for PD measurement. Digital PD tools can come close: a 2024 study found the Eye Measure app differed from a pupillometer by -0.59 mm on average for distance IPD. The key advantage of digital tools is consistency across staff and the ability to support remote measurements, while pupillometers offer the highest precision for in-person fittings.
What role does AI play in digital PD measurement?
In PD measurement, AI primarily functions as computer vision: it detects eye landmarks, scores image quality, and flags captures with poor lighting or alignment. This helps reduce measurement errors caused by inconsistent positioning. AI does not replace the need for proper capture technique and good lighting.
Are digital PD measurements accurate enough for progressive lenses?
Progressive lenses require both PD and segment height measurements, and tolerances are tighter because lens corridors are narrow. While digital PD tools can provide acceptable PD accuracy, the overall fitting for progressives also depends on segment height, frame tilt, and vertex distance. Many practices use digital PD tools as one input in a multi-measurement workflow for progressives rather than relying on a single capture.
What should I look for when choosing a digital PD tool for my practice?
Look for published validation data (not just marketing claims), clear capture guidance for patients and staff, a reliable scaling reference (credit card, printed marker, or known frame dimensions), quality scoring that flags unreliable captures, and integration with your existing ordering or POS system. Test any tool against your pupillometer baseline before committing.
Can patients measure their own PD at home with a digital tool?
Yes, several apps support patient self-measurement for remote eyewear orders. However, accuracy depends on the patient following capture instructions carefully. The 2023 Cureus study found that app accuracy varied widely, with some apps achieving 0.51 mm MAE while others showed 1.38 mm. Practices offering remote PD capture should choose validated apps and build in a verification step for measurements that fall outside expected ranges.

I am a seasoned software engineer with over two decades of experience and a deep-rooted background in the optical industry, thanks to a family business. Driven by a passion for developing impactful software solutions, I pride myself on being a dedicated problem solver who strives to transform challenges into opportunities for innovation.